koyaaniskatsi (from the hopi language) n. 1. crazy life. 2. life in
turmoil. 3. life disintegrating. 4. life out of balance. 5. a state of life
that calls for another way of living.
From the dust jacket of the Philip Glass album Koyaaniskatsi
September 4 2003 - Something is terribly wrong with the way some criminal justice authorities
have begun to enforce the law against physicians and pharmacists who
prescribe and dispense high dose opioids to treat chronic pain. The
necessary balance in pain policy described by David Joranson and June Dahl
of the University of Wisconsin has tipped drastically in the direction of
ruthless drug control and away from compassionate collaboration. This is a
recent development. The past five years has generated an unprecedented list
of health care providers charged with murder for allegedly providing
inappropriately large quantities of opioids to pain patients.
In Kansas, Dr. Stan Naramore was convicted of murdering one patient and
attempting the murder of another, but his conviction was overturned on
appeal. Murder charges were filed against Indiana physician Jong Bek, and
later dropped for lack of evidence. Dr. Robert Weitzel of Salt Lake City was
charged with first-degree murder and convicted of manslaughter and negligent
homicide, then acquitted on retrial. In California, five charges of
first-degree murder were brought against Dr. Frank Fisher, Pharmacist
Stephen Miller, and Miller's wife Madeline Miller, but were dismissed four
years later due to lack of evidence. These are the happy-ending stories.
Dr. James Graves of Pace, Florida, charged with murder and convicted of
manslaughter, now waits in prison for his appeal to be heard. Murder charges
have been filed against Florida physician Denis Deonarine, Dr. Spurgeon
Green from Georgia, and Dr. Jesse Benjamin Henry from Albuquerque (as well
as Hong Lu Henry, Dr. Henry's wife). Other physicians and pharmacists have
been charged with lesser crimes resulting from their prescribing or
dispensing of opioid analgesics.
This is drug control policy out of balance. It creates a "chilling effect"
on the prescribing and dispensing of opioids for legitimate pain patients.
It is a state of regulation that calls for a different way of regulating.
Balance is an appealing concept in everyday life. Most people try to balance
work with family, personal concerns with social concerns, and present needs
with future needs. Achieving balance is a familiar activity.
Scientists try to balance the likelihood of two errors. Type I error occurs
when a hypothesis is considered proven, but in fact it is false. Type II
error occurs when a hypothesis is considered unproven, but in fact it is
true. The more one attempts to reduce the probability of Type I error, the
more one increases the probability of Type II error, and vice-versa. The sum
of the two errors is minimized when they are balanced, not when the
avoidance of one is emphasized over avoidance of the other.
The result is similar in law enforcement, because it is impossible to know
in advance whether high dose opioid prescriptions have been issued or
dispensed for a legitimate medical purpose. There is no laboratory value or
diagnostic image that can confirm pain. The threat of strong law enforcement
can prevent many drug diverters from accessing medications, but many
legitimate patients will also be denied. Behaviors designed to reduce the
error of providing controlled substances to drug diverters will increase the
error of refusing controlled substances to legitimate pain patients.
It is interesting to note that the "red flags" used by regulators to
identify inappropriate controlled substance prescribing and dispensing, are
in many ways similar or identical to the criteria health care providers use
in identifying appropriate pain management practice. The difference
perception of these factors can lead to imbalance.
Consider the ambiguity of these red flags:
-
Patient comes from a long distance.
Regulators become concerned when
patients travel many hundreds of miles to a receive prescriptions for
opioids. They wonder why patients don't just get their medications in their
own community. But as the specialty of pain management emerges, and as
primary care practitioners are encouraged to refer pain patients to
specialists, it becomes increasingly more common to refer pain patients to
physicians who may be a considerable distance from the patient's home.
-
Large quantity of controlled substances prescribed.
The prescribing of
large quantities of opioids will attract regulatory attention to any
physician, and it probably should. Regulators may claim to be unaffected by
high volume, but that is not the reality of the current regulatory climate.
In health care, however, a high volume of opioids for pain patients is a
badge of honor among those who truly do what is right to meet the needs of
those who suffer.
-
The dose is potentially lethal.
Regulators may become concerned with
large doses that would kill an opiate naive patient. Yet, health care
providers recognize that analgesic tolerance may require increasing doses to
as high a level as is needed to achieve analgesia without intolerable side
effects. Drugs don't have doses, patients have doses.
- The patient asked for drugs by name.
To a regulator, it will seem
suspicious that a pain patient refuses medications that are not controlled
substances and insists that only specific opiates will work. This is the
sign of a "drug seeker." A health care provider will appreciateknowing what
drugs a documented pain patient has found, through experience, to be safe
and effective for that patient. There is no need to again try those drugs
that have not worked in the past.
-
The doctor prescribes whatever the patients want.
To a regulator it will
seem suspicious that a physician will prescribe based on the patient's
expressed needs rather on objective clinical findings. But health care
providers are moving in the direction of learning the patient's functional
goals and trying to meet those goals. A successful health care practice
focuses on the patients' quality of life, not on objective clinical
findings.
- Patients return too early.
It is alarming to regulators that a patient
who has received a thirty-day of supply of medication may run out of
medication early and return before thirty days, without an appointment, to
receive additional medication. Health care providers know that a health
crisis cannot be scheduled, and that patients whose condition suddenly
worsens must be seen immediately. A gap in treatment may send the patient
into a downward spiral or may force the patient to use non-medical street
drugs to obtain relief.
- The patient is directed to use multiple pharmacies.
For a regulator,
the fact that a patient has been told to go to several different pharmacies
may be seen as suspicious, and it should be. On the other hand, in a
community where pharmacists are frightened by law enforcement and are
reluctant to dispense large quantities of opioids, the only choice may be to
use several pharmacies to obtain the required amount of medication.
- Many different drugs are being prescribed.
The prescribing and
dispensing of many different controlled substances for seemingly unrelated
conditions will signify to regulators the possibility of drug diversion
rather than legitimate medical care. In pain management, however, health
care providers realize that anxiety, insomnia, and depression are
accompanying conditions that require additional pharmacological treatment to
meet the patients' needs.
All of these red flags have alternative meanings, based on the perspective
of either a drug control regulator or a pain management professional. To a
drug control regulator they are signs that something is going wrong. To a
health care provider they are signs that things are going right. Discerning
the reality of whatever these red flags suggest requires drug control
regulators and health care providers to go beyond mere "indicators" and talk
openly with each other. Unfortunately, the culture of law enforcement does
not lend itself well to open dialogue. Law enforcement is trained to conduct
discreet surveillance, gather evidence, and then use massive force when the
time is right. Early dialogue looks to them too much like teaching criminals
how to not get caught. Health care providers are also skittish about early
dialogue. A legacy of suspicion and distrust makes them reluctant to draw
attention to themselves and perhaps implicate themselves in wrong doing by
contacting law enforcement.
A system must be developed to facilitate early dialogue so that ambiguous
red flags are clarified. This system would include consults between law
enforcement officers and specific health care providers who are under
suspicion, as well as consults with expert peer reviewers with knowledge of
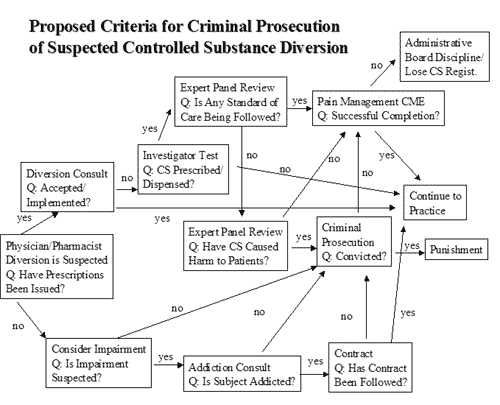
practice standards. The following flow chart describes one such possible
system. I would welcome comments about the flow chart from anyone.
David Brushwood is Professor of Pharmacy Health Care Administration at the
University of Florida in Gainesville. He is a Mayday Scholar with the
American Society of Law, Medicine and Ethics (ASLME).
For information about ASLME pain policy projects, go to ASLME.




